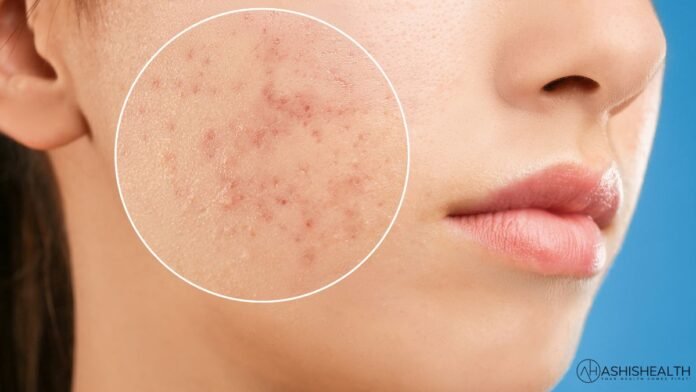
Acne is a common skin condition that affects millions of individuals worldwide, transcending age, gender, and ethnic backgrounds. Characterized by the presence of pimples, blackheads, whiteheads, and often, painful cysts, acne arises from the clogging of hair follicles with oil and dead skin cells. This dermatological concern typically manifests during adolescence, as hormonal changes stimulate the sebaceous glands to produce excess oil. However, acne can persist into adulthood and may be influenced by various factors, including genetics, diet, stress, and environmental elements. Beyond its physical impact, acne can have profound effects on an individual’s emotional well-being, self-esteem, and overall quality of life, making it a multifaceted challenge that extends beyond mere skin deep. Understanding the causes, triggers, and available treatment options is crucial for managing and mitigating the impact of acne on both physical and mental health.
What are the different types of acne?
Acne manifests in various forms, each characterized by specific lesions and severity levels. The main types of acne include:
Comedones
Blackheads: Open comedones that appear as small, dark spots on the skin’s surface. The dark color is due to the oxidation of the trapped sebum (oil) and dead skin cells.
Whiteheads: Closed comedones that are small, flesh-colored bumps. They occur when a hair follicle is completely blocked, preventing the oxidation of sebum.
Inflammatory Acne
Papules: Small, red bumps that may be tender to the touch.
Pustules: Pimples with a white or yellow center caused by pus accumulation. They are often surrounded by red, inflamed skin.
Nodules: Larger, painful lumps beneath the surface of the skin. Nodules can be deep-seated and may cause scarring.
Cysts: Severe, painful lesions filled with pus. Cysts are deep and may lead to scarring. Professional medical intervention is often required for cystic acne.
Other Types
Acne Conglobata: A severe and rare form of acne characterized by interconnected nodules and abscesses. It can cause extensive scarring.
Acne Fulminans: An abrupt onset of severe acne, often accompanied by systemic symptoms such as fever and joint pain.
Gram-Negative Folliculitis: A bacterial infection that can develop from long-term antibiotic use for acne.
Hormonal Acne
Some individuals, especially women, may experience acne flare-ups due to hormonal fluctuations. Hormonal acne often appears on the lower face, jawline, and neck.
Understanding the specific type of acne is crucial for determining an effective treatment plan. Consulting with a dermatologist can help identify the underlying causes and tailor a regimen to address the individual’s unique skin condition.
What are the symptoms of acne?
Acne presents a range of symptoms, and the severity can vary from mild to severe. Common symptoms of acne include:
Lesions
Comedones: Blackheads and whiteheads are the earliest and mildest forms of acne lesions.
Papules: Small, red bumps that may be tender to the touch.
Pustules: Pimples with a white or yellow center caused by pus accumulation.
Nodules: Large, painful lumps beneath the surface of the skin.
Cysts: Deep, painful, and often filled with pus.
Inflammation
Redness and inflammation around acne lesions.
Pain and Tenderness
Acne lesions, especially nodules and cysts, can be painful and tender.
Scarring
Severe forms of acne, such as nodules and cysts, can lead to permanent scarring.
Changes in Skin Texture
Uneven skin texture due to the presence of acne lesions.
Oily Skin
Excessive oil (sebum) production, especially in the T-zone (forehead, nose, and chin).
Hyperpigmentation
Dark spots or discoloration left behind after an acne lesion heals.
Hormonal Fluctuations
Acne may worsen during hormonal changes, such as puberty, menstrual cycles, pregnancy, or menopause.
Itching
Some individuals may experience itching around acne lesions.
Psychological Impact
Acne can have psychological symptoms, including lowered self-esteem, anxiety, and depression, especially in more severe cases.
It’s essential to note that symptoms can vary from person to person, and some individuals may have a few isolated pimples, while others may experience more widespread and severe forms of acne. Seeking professional advice from a dermatologist is recommended for proper diagnosis and tailored treatment options based on individual skin conditions.
What causes acne?
Acne develops when hair follicles in the skin become clogged with oil and dead skin cells. The primary factors contributing to the formation of acne include:
Excess Oil Production (Sebum)
Hormonal changes, particularly during puberty, can stimulate the sebaceous (oil) glands to produce more oil (sebum). This excess oil can mix with dead skin cells and plug hair follicles.
Clogged Hair Follicles
The combination of excess oil and dead skin cells can lead to the formation of comedones, including blackheads and whiteheads, which are the basic building blocks of acne lesions.
Bacteria (Propionibacterium acnes)
The bacterium P. acnes, naturally present on the skin, can proliferate within clogged hair follicles. This leads to inflammation and the formation of inflammatory acne lesions like papules, pustules, nodules, and cysts.
Hormonal Changes
Hormonal fluctuations, common during adolescence, menstruation, pregnancy, and the use of oral contraceptives, can influence oil production. Androgens, a type of hormones, play a significant role in stimulating sebum production.
Genetics
A family history of acne may increase the likelihood of developing the condition. Genetic factors can influence how the skin responds to hormonal changes and how prone it is to inflammation.
Diet
While the direct link between diet and acne is still a subject of research, some studies suggest that certain dietary factors, such as high glycemic index foods and dairy products, may contribute to acne development in some individuals.
Stress
Stress can trigger hormonal changes that may exacerbate acne. Additionally, stress may lead to behaviors that worsen acne, such as picking or scratching the skin.
Cosmetics and Skin Care Products
Certain cosmetic and skin care products may contain ingredients that can clog pores and contribute to acne. It’s important to choose non-comedogenic products.
Friction and Pressure
Friction from tight clothing, helmets, or backpacks can aggravate acne, especially in areas prone to breakouts.
Environmental Factors
Exposure to environmental pollutants and humid conditions can contribute to acne development.
It’s crucial to recognize that acne is a multifactorial condition, and different individuals may be affected by a combination of these factors. Effective management often involves a personalized approach that considers the specific causes and characteristics of an individual’s acne. Seeking guidance from a dermatologist can help in formulating an appropriate treatment plan.
What are the risk factors for developing acne?
Several factors can increase the risk of developing acne. These risk factors may vary among individuals, and the interplay of multiple factors often contributes to the onset and severity of acne. Common risk factors include:
Age and Puberty
Acne is most prevalent during adolescence when hormonal changes are significant. Puberty triggers an increase in androgen hormones, leading to heightened sebum production and an increased risk of acne.
Hormonal Changes
Hormonal fluctuations related to the menstrual cycle, pregnancy, and the use of oral contraceptives can influence the development of acne. Conditions like polycystic ovary syndrome (PCOS) associated with hormonal imbalances may also contribute.
Family History (Genetics)
Having close relatives, such as parents or siblings, with a history of acne increases the likelihood of developing the condition. Genetic factors play a role in how the skin responds to hormonal changes and inflammation.
Gender
While acne is common in both males and females, males may experience more severe forms, especially during adolescence. Hormonal changes unique to each gender can impact the development of acne.
Cosmetic and Hair Products
Certain cosmetics and hair care products may contain ingredients that can contribute to pore clogging, increasing the risk of acne. Using non-comedogenic products is advisable.
Dietary Factors
While the link between diet and acne is complex and varies among individuals, some studies suggest that diets high in refined carbohydrates and dairy may influence acne development in certain people.
Stress
Stress doesn’t directly cause acne, but it can exacerbate existing conditions. Stress triggers hormonal changes that may contribute to increased sebum production and inflammation.
Occupational and Environmental Factors
Exposure to certain occupational or environmental factors, such as pollutants and high humidity, may contribute to acne development.
Friction and Pressure
Constant friction or pressure on the skin, such as from tight clothing, helmets, or leaning on the face, can contribute to the formation of acne.
Previous Acne or Acne Flare-ups
Individuals with a history of acne may be more prone to future breakouts. Additionally, unresolved or improperly treated acne lesions can contribute to scarring and an increased risk of new lesions.
Understanding these risk factors can help individuals take preventive measures and adopt appropriate skincare practices. If acne is a persistent concern, consulting with a dermatologist can provide personalized guidance and treatment options.
Diagnosis and Tests
In most cases, a dermatologist can diagnose acne based on a physical examination of the skin and a discussion of the individual’s medical history. No specific tests are usually required for a straightforward diagnosis of acne. However, in certain situations, or if there are concerns about underlying conditions, a dermatologist may perform additional assessments or tests. Here are some aspects of the diagnostic process for acne:
Physical Examination
The dermatologist will examine the skin, looking for different types of lesions, their distribution, and any signs of inflammation. This examination helps in determining the severity of the acne and the appropriate treatment approach.
Medical History
Information about the individual’s medical history, including past and current skin conditions, family history of acne, medications, and lifestyle factors, is crucial for understanding the context of the acne and identifying potential triggers.
Grading and Classification
Acne is often graded based on its severity, ranging from mild to severe. The dermatologist may also classify the type of acne lesions present, such as comedones, papules, pustules, nodules, or cysts.
Exclusion of Other Conditions
Sometimes, other skin conditions may mimic acne. The dermatologist may rule out conditions like rosacea, folliculitis, or perioral dermatitis through careful examination.
Hormonal Evaluation
In cases where hormonal factors are suspected, especially in adult women, the dermatologist may consider hormonal evaluation. This can involve blood tests to measure hormone levels, such as androgens.
Culture or Biopsy (Rare Cases)
In rare cases, a dermatologist may perform a culture or biopsy to rule out bacterial infections or other skin disorders. This is not a routine procedure for typical acne cases.
It’s important to note that the diagnostic process may vary depending on the individual’s unique situation. Acne is a common and usually straightforward condition to diagnose, and treatment often begins with over-the-counter or prescription topical medications. If acne is severe or persistent, or if there are concerns about underlying health issues, a dermatologist’s expertise is invaluable for accurate diagnosis and a tailored treatment plan.
Acne Management and Treatment
The management and treatment of acne aim to reduce symptoms, prevent new lesions from forming, and minimize the risk of scarring. The approach to treatment depends on the severity of the acne and individual factors. Here are various strategies and interventions commonly employed for managing acne:
Topical Treatments
Retinoids: Derived from vitamin A, these help unclog pores and prevent the formation of new lesions.
Topical Antibiotics: These reduce the population of Propionibacterium acnes (P. acnes) bacteria on the skin, helping to decrease inflammation.
Benzoyl Peroxide: An antimicrobial agent that can reduce bacteria and help prevent the formation of new lesions.
Oral Medications
Oral Antibiotics: In cases of moderate to severe inflammatory acne, oral antibiotics may be prescribed to reduce bacteria and inflammation.
Oral Contraceptives: For females, hormonal contraceptives containing estrogen and progestin can help regulate hormonal fluctuations and improve acne.
Isotretinoin (Accutane): Reserved for severe, nodular acne, isotretinoin is a powerful oral medication that reduces oil production and prevents acne formation. It requires careful monitoring due to potential side effects.
Combination Therapies
Dermatologists often recommend combination therapies, such as using both topical and oral medications, to address multiple aspects of acne.
Lifestyle and Skincare
Gentle Cleansing: Using a mild cleanser and avoiding harsh scrubbing can help prevent irritation.
Avoiding Picking or Squeezing: Picking at acne lesions can worsen inflammation and increase the risk of scarring.
Non-comedogenic Products: Using skincare and cosmetic products labeled as “non-comedogenic” helps prevent pore-clogging.
Sun Protection: Sunscreen is essential to protect the skin, and some acne medications may increase sensitivity to sunlight.
Procedural and Physical Treatments
Chemical Peels: Dermatologists may use chemical peels to exfoliate the skin and reduce the appearance of mild acne.
Laser and Light Therapy: These treatments can target bacteria, reduce inflammation, and promote skin healing.
Extraction and Drainage
Dermatologists may perform extraction or drainage of large cysts to relieve pain and reduce the risk of scarring.
Maintenance Therapy
After achieving control over acne, individuals may need ongoing maintenance therapy to prevent new breakouts.
It’s important to consult with a dermatologist to determine the most suitable treatment plan based on the type and severity of acne, as well as individual factors such as skin type and medical history. Consistency in treatment and follow-up appointments is crucial for effective acne management. Additionally, patience is key, as improvement may take time, and adjustments to the treatment plan may be necessary.
How can I make my acne go away at home?
While more severe cases of acne may require professional medical intervention, there are several home care practices that can help manage and improve mild to moderate acne. Here are some tips for managing acne at home:
Gentle Cleansing
Wash your face twice a day using a mild, fragrance-free cleanser. Avoid harsh scrubbing, as it can irritate the skin and exacerbate acne.
Non-comedogenic Products
Use skincare and cosmetic products labeled as “non-comedogenic” to reduce the risk of pore-clogging.
Hydration
Stay well-hydrated by drinking plenty of water. Hydration is essential for overall skin health.
Avoid Picking or Squeezing
Resist the temptation to pick or squeeze acne lesions, as this can lead to scarring and worsen inflammation.
Sun Protection
Use a broad-spectrum sunscreen with SPF 30 or higher to protect your skin from the sun. Some acne medications may increase sensitivity to sunlight.
Topical Treatments
Over-the-counter topical treatments containing benzoyl peroxide, salicylic acid, or alpha hydroxy acids can help reduce mild acne. Follow the product instructions carefully.
Tea Tree Oil
Tea tree oil has natural antibacterial properties. Dilute it with a carrier oil (such as jojoba or coconut oil) and apply it to affected areas, but be cautious, as it may cause irritation in some individuals.
Honey and Cinnamon Mask
Mix honey and cinnamon to form a paste and apply it to the face. Leave it on for about 10-15 minutes before rinsing. Some people find this home remedy beneficial.
Avoiding Irritants
Avoid harsh skincare products, excessive sun exposure, and irritating fabrics. Be mindful of potential triggers that can worsen acne.
Healthy Diet
While the relationship between diet and acne is complex, maintaining a balanced and healthy diet can contribute to overall skin health. Consider reducing the intake of high-glycemic foods and dairy if you suspect a connection with your acne.
Remember, results may take time, and consistency is key. If your acne persists or worsens despite home care efforts, or if you experience severe acne, scarring, or emotional distress, it’s advisable to seek professional advice from a dermatologist. They can provide a tailored treatment plan based on your specific skin condition and needs.
Preventing acne
While it may not be possible to completely prevent acne, adopting certain lifestyle and skincare practices can help minimize the risk of breakouts. Here are some tips for preventing acne:
Gentle Cleansing
Wash your face twice a day using a mild, fragrance-free cleanser. Avoid overwashing or using harsh scrubs, as this can irritate the skin and potentially worsen acne.
Non-comedogenic Products
Use skincare and cosmetic products labeled as “non-comedogenic” to reduce the likelihood of pore-clogging.
Hydration
Stay well-hydrated by drinking enough water throughout the day. Proper hydration supports overall skin health.
Healthy Diet
Maintain a balanced and nutritious diet rich in fruits, vegetables, whole grains, and lean proteins. While the direct link between diet and acne is still being studied, a healthy diet can contribute to overall skin health.
Limit High-Glycemic Foods
Some studies suggest that a diet high in refined carbohydrates and sugary foods may be associated with an increased risk of acne. Consider reducing the intake of such foods.
Manage Stress
Chronic stress can contribute to hormonal changes that may worsen acne. Practice stress-reduction techniques such as meditation, deep breathing, or yoga.
Regular Exercise
Engage in regular physical activity to promote overall well-being. Exercise increases blood flow, which can contribute to healthier skin.
Sun Protection
Use a broad-spectrum sunscreen with SPF 30 or higher to protect your skin from the sun. Some acne medications can increase sensitivity to sunlight.
Hands Off
Avoid touching your face throughout the day, as this can transfer oils, dirt, and bacteria to your skin.
Shower After Sweating
If you engage in activities that cause you to sweat, such as exercising, make sure to shower afterward to remove sweat and prevent pore-clogging.
Hormonal Considerations
For individuals with hormonal acne, especially adult women, hormonal therapies such as oral contraceptives or anti-androgen medications may be considered under the guidance of a healthcare professional.
Regular Dermatologist Visits
Regular check-ups with a dermatologist can help identify potential acne triggers, and a dermatologist can provide guidance on an effective skincare routine and recommend appropriate treatments if necessary.
It’s important to note that everyone’s skin is unique, and what works for one person may not work for another. If you’re struggling with acne or have concerns about your skin, consulting with a dermatologist can provide personalized advice and treatment options tailored to your specific needs.
The Bottom Line
The bottom line is that while it may not be possible to entirely prevent acne, adopting a consistent and gentle skincare routine, maintaining a healthy lifestyle, and seeking professional advice when needed can significantly reduce the risk of breakouts and contribute to overall skin health. Personalized approaches, such as using non-comedogenic products, managing stress, and staying hydrated, can be key components in preventing and managing acne effectively. If acne persists or becomes a concern, consulting with a dermatologist is recommended for a tailored treatment plan and expert guidance.